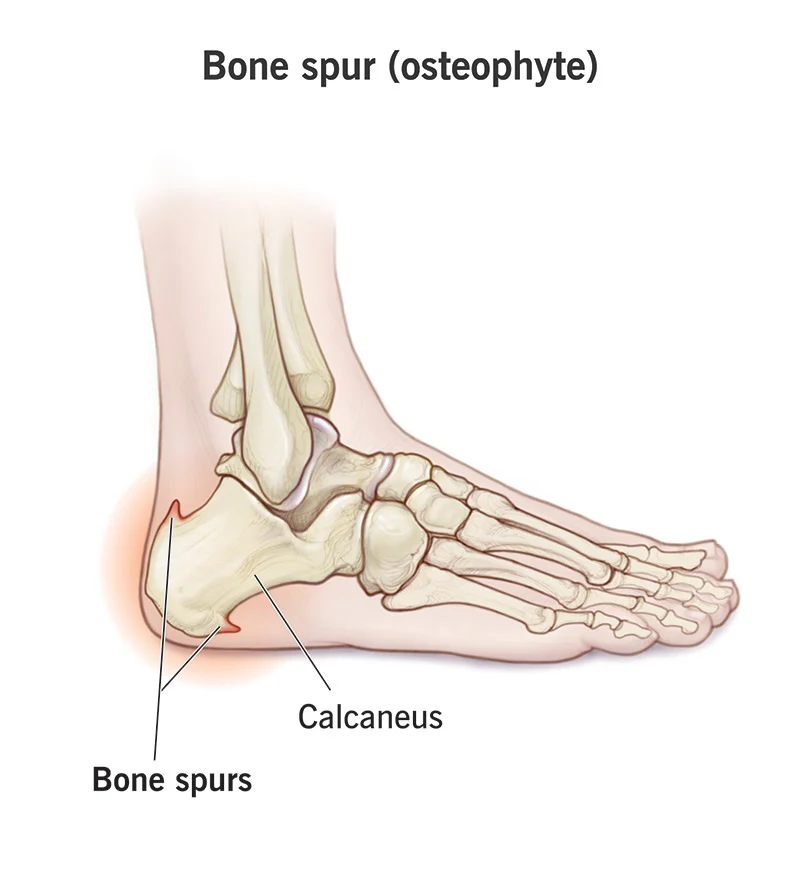
A heel spur (calcaneal spur) is a bony outgrowth on the heel bone caused by long-term stress, muscle strain, or repeated tearing of the membrane covering the heel bone. Often associated with plantar fasciitis, symptoms include sharp heel pain, though many are painless. Treatments focus on reducing inflammation through rest, orthotics,physiotherapy and medication. Evidence based practices indicates that full recovery occurs with physiotherapy within 15 sessions.
- Chronic Stress Mechanism: Continuous stress on foot ligaments and tendons (often due to obesity, improper footwear, or overactivity) causes the plantar fascia to pull away from the heel bone.
- Inflammation and Repair: This chronic strain causes tears in the periosteum (the membrane covering the bone). As the body attempts to repair this damage, it deposits calcium, creating a bony projection.
- Associated Conditions: Frequently associated with plantar fasciitis, but a spur itself does not always cause pain.
- Structure: Simple spurs are triangular and sharp, while irregular spurs have less-defined borders.
- Risk Factors: Increased age, higher BMI, prolonged standing on hard surfaces, and high arches (pes cavus) or severe flat feet.
Clinical Features
- Pain Characteristics: Sharp, piercing, or stabbing pain on the bottom of the heel, often described as walking on a nail or pin.
- Timing of Pain: Pain is characteristically worst with the first few steps in the morning or after prolonged sitting (post-static dyskinesia).
- Activity Factors: Pain may reduce after initial walking but increase after long periods of standing, walking, or running.
- Tenderness: Intense, localized tenderness when applying direct pressure to the center of the heel pad.
- Physical Appearance: While the spur is internal, chronic cases may show localized swelling or inflammation.
- Asymptomatic Spikes: Many spurs are found incidentally on imaging and cause no pain at all.
- Plantar Fasciitis: Inflammation of the connective tissue on the sole of the foot is the most common cause of associated pain.
- Achilles Tendinitis: Dorsal spurs can cause pain at the back of the heel where the Achilles tendon attaches.
- Gait Changes: Patients may alter their walking gait to avoid putting pressure on the heel.
Assessment:
A physiotherapy assessment for a calcaneal (heel) spur focuses on evaluating chronic heel pain, often associated with plantar fasciitis, through history-taking, gait analysis, and physical tests. Key components include palpation for tenderness, assessing calf/plantar fascia flexibility, and checking for biomechanical issues like flat feet.
- History Taking: Evaluates the nature of pain (e.g., sharp pain with first steps in the morning), duration, previous injuries, footwear choices, and occupational strain.
- Physical Examination:
- Palpation: Checking for tender spots on the medial tubercle of the calcaneus, where plantar spurs typically form.
- Mobility Testing: Assessing joint range of motion (ROM), particularly ankle dorsiflexion, to identify tight calf muscles (gastrocnemius and soleus).
- Functional Testing: Observing gait (walking patterns) to check for abnormalities.
- Differential Diagnosis: Ensuring symptoms are not from Achilles tendinitis (if a posterior spur is present), fat pad atrophy, or neurological issues like tarsal tunnel syndrome.
- Imaging Referral: While physical examination is key, therapists may recommend or refer for x-rays to confirm the bony outgrowth and ultrasound to assess the soft tissue inflammation around the spur.
- Pain reduction when weight is removed.
- Significant tenderness on the plantar medial heel.
- Tightness in the plantar fascia and Achilles tendon.
Physiotherapy treatment for calcaneal spurs (heel spurs) focuses on reducing inflammation, relieving pain, and addressing the underlying biomechanical issues, such as tight calf muscles or improper foot mechanics.
- Plantar Fascia and Calf Stretching
- Description: Stretching the calf muscles (gastrocnemius and soleus) and the plantar fascia helps reduce tension on the heel bone.
- Examples: Calf stretches against a wall, towel stretches for the foot, and plantar fascia stretches (pulling toes back toward the shin).
- 2.Joint Mobilization: Techniques targeting the subtalar and ankle joints to increase range of motion,Gait and Postural Training: Correcting the way a patient walks to prevent future injuries
3.Manual Therapy and Deep Tissue Massage
Description: A therapist applies deep pressure to the sole of the foot and calf muscles to release myofascial trigger points.
Technique: Massage can increase blood circulation, promote healing, and relax tight muscles, often using techniques like cross-frictional massage on the plantar fascia.
Ice Therapy / Cryotherapy
Description: Applying cold to the heel reduces inflammation and numbs the pain.
Method: Rolling a frozen water bottle or a golf ball under the foot for 10–15 minutes, several times a day.
Strengthening Exercises for Foot Intrinsic Muscles
Description: Strengthening the small muscles in the foot supports the arch and reduces strain on the heel.
Examples: Towel scrunches (using toes to grab a towel) and picking up marbles with toes.
Taping and Orthotic Support
Description: Kinesiology tape can be applied to support the arch, while orthotic inserts or heel cups are used to reduce shock and pressure on the spur.
Goal: Immediate pain relief during daily activities.
Ultrasound Therapy
Description: Therapeutic ultrasound uses sound waves to increase blood flow and raise the temperature of the tissue, helping to decrease muscle tension and inflammation.
Night Splints
Description: A splint is worn while sleeping to keep the foot in a slightly flexed position, which prevents the plantar fascia from shortening and reduces pain with the first step in the morning.