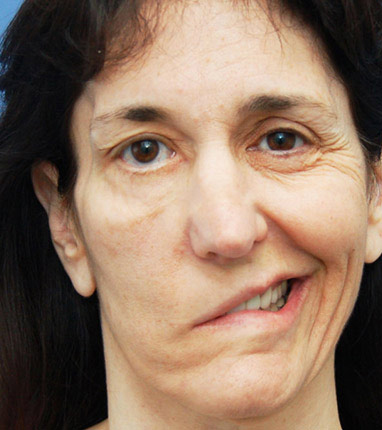
Bell’s palsy is a leading reason people suddenly lose movement on one side of their face. It usually shows up when the facial nerve gets irritated or swollen, often after a viral infection like the one that causes cold sores. When that nerve can’t properly send messages from the brain to the muscles, things like smiling, blinking, or even closing your eye can become difficult. The symptoms tend to come on fast, sometimes within just a day or two.
Facial paralysis (also called facial palsy) is a broader term that describes the loss of voluntary muscle movement in the face due to nerve damage or dysfunction. Unlike Bell’s palsy, which is idiopathic (meaning it arises without a known cause), facial paralysis can result from a variety of known conditions. These may include trauma, infections, tumors, neurological disorders, or strokes. Ramsay Hunt Syndrome, for example, is another viral cause of facial paralysis but is not the same as Bell’s palsy. In these cases, identifying the underlying cause is key to determining the right treatment.Bell’s palsy is a form of facial palsy, but not all facial palsy is Bell’s palsy. Facial palsy refers to any weakness or paralysis of the facial muscles caused by damage to the facial nerve. Bell’s palsy, on the other hand, is the most common type of facial palsy and typically occurs without a known cause, though viral infections are often suspected.
Think of facial paralysis as the umbrella term: Bell’s palsy is just one possible diagnosis underneath it. Bell’s palsy refers specifically to sudden-onset, idiopathic facial paralysis, often presumed to be viral. Facial paralysis, more broadly, refers to the symptom itself and can stem from many sources.
- Bell’s Palsy: A specific type of facial paralysis with no clearly identifiable cause, often linked to viral inflammation.
- Facial Paralysis: A general term describing facial nerve weakness, which can result from known conditions like injury, infection, stroke, or tumors.
CAUSES OF BELL’S PALSY
Bell’s palsy is considered idiopathic, meaning its exact cause is unknown. However, many cases are believed to be triggered by a viral infection, especially herpes simplex virus (HSV-1), the virus responsible for cold sores. Other potential viral links include:
- Epstein-Barr virus
- Cytomegalovirus
- Influenza
These viruses may cause inflammation and swelling of the facial nerve, disrupting communication between the brain and facial muscles.
CAUSES OF FACIAL PALSY
Facial palsy can result from a wide variety of known medical issues, including:
- Viral infections (e.g., herpes zoster, Lyme disease, Epstein-Barr)
- Bacterial infections (e.g., ear infections)
- Neurological conditions (e.g., multiple sclerosis)
- Stroke or brain tumor
- Facial trauma or surgical injury
- Congenital disorders
Each of these can damage the facial nerve, leading to either temporary or permanent muscle weakness on one or both sides of the face.
Bell’s palsy usually appears suddenly, often within 48 hours. Common symptoms include:
- Sudden weakness or paralysis on one side of the face
- Drooping of the mouth or eyelid
- Inability to close the affected eye
- Loss of taste on the front part of the tongue
- Increased sensitivity to sound in one ear
- Dry eye or mouth on the affected side
- Headache or mild ear pain
The signs of facial palsy depend on its underlying cause but may include:
- Drooping on one or both sides of the face
- Difficulty closing the eye or mouth
- Drooling
- Reduced ability to smile, frown, or raise eyebrows
- Changes in tear and saliva production
- Altered taste sensation
- Headache or ear pain
Although Bell’s palsy can be a frightening condition, the good news is that numerous treatments exist to aid in recovery. Treatment aims to lower nerve inflammation, ease symptoms, and encourage the comeback of face muscular control.
- Antibiotics for bacterial infections
- Surgical intervention to remove tumors or decompress nerves
- Rehabilitation and therapy for stroke or neurological disorders
- Ongoing management for chronic conditions like MS
- PHYSIOTHERAPY IN BELL'S PALSY AND FACIAL PALSY
- Physiotherapy for Bell’s palsy focuses on stimulating the facial nerve, preventing muscle contractures, and restoring facial symmetry through tailored exercises, manual therapy, and electrical stimulation. Key interventions include mirror exercises, facial massages, and neuromuscular retraining.
- Facial Exercises & Mime Therapy: Targeted, gentle movements performed in front of a mirror (e.g., raising eyebrows, smiling, closing eyes, puckering lips) to retrain weak muscles.
- Neuromuscular Retraining (NMRT): Specialized, repetitive exercises designed to break poor habits and re-establish correct muscle activation patterns to reduce synkinesis (unwanted co-contractions).
- Mirror Therapy: Performing exercises while observing the face in a mirror to provide visual feedback, enhancing the brain's ability to coordinate and correct facial movements.
- Manual Therapy & Massage: Soft tissue massage techniques (effleurage, kneading) on the affected side to improve circulation, decrease stiffness, and reduce pain.
- Electrical Stimulation (EMS): Using low-level stimulation (Galvanic or Faradic) to trigger muscle contractions, preventing atrophy, and maintaining muscle tone during the acute, paralyzed phase.
- Kinesio Taping: Application of specialized tape to the face to support weakened muscles, encourage better alignment, and provide sensory stimulation.
- Proprioceptive Neuromuscular Facilitation (PNF/Kabat Method): A manual technique involving resistance applied to specific facial areas to stimulate muscular contraction and movement, often working from the stronger side to the weaker.
- Eye Care & Protection (Adjunct Care): Education on taping the eye closed at night and using moisturizing drops to prevent corneal ulcers when the eyelid cannot close properly.
- Additional Recommendations:
- Lifestyle Modification: Using a straw to assist with drinking and chewing on the affected side to strengthen masseter muscles.
- Early Intervention: Starting exercises early can improve long-term outcomes and reduce the risk of chronic sequelae.
- Avoid Overworking: Exercises should be done in sets (e.g., 10 repetitions) to prevent fatiguing the weak muscles.