Introduction
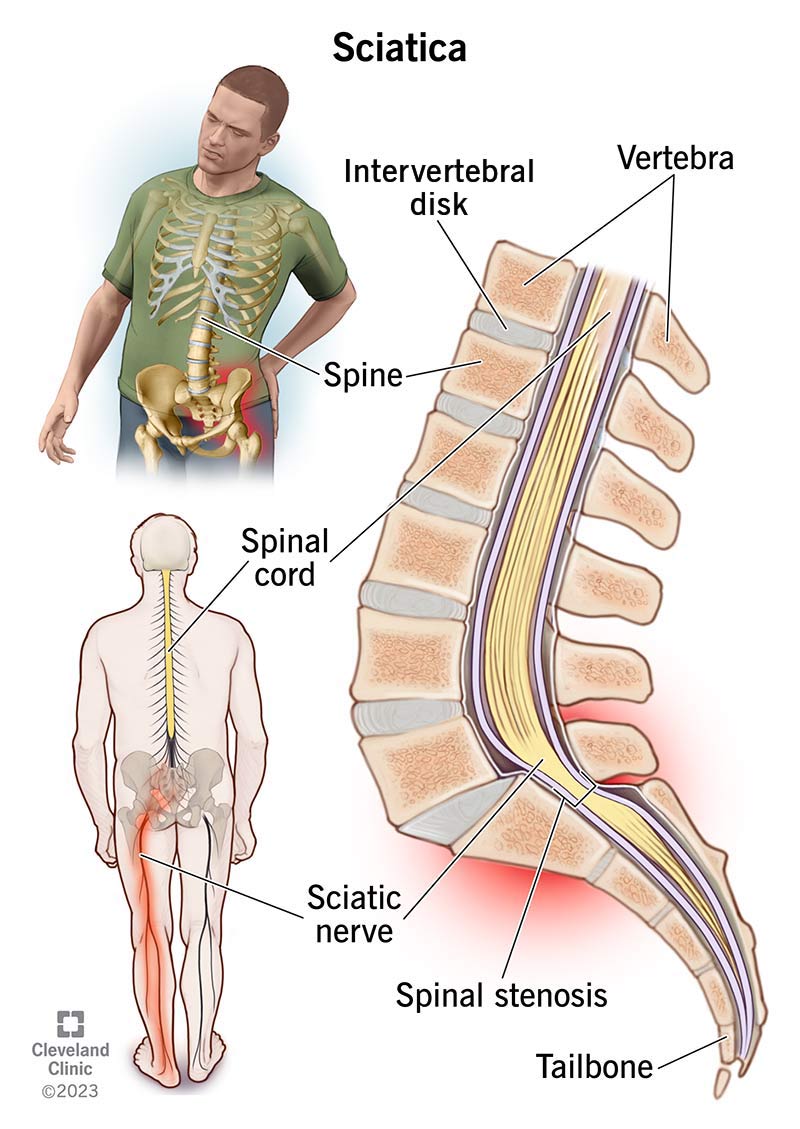
Sciatica refers to radiating pain or paresthesias along the course of the sciatic nerve from the lower back or buttock to one or both legs or an associated lumbosacral nerve root. While it may be common to refer to any low back pain or radicular leg pain as sciatica, it is important to note that sciatica entails pain directly resulting from sciatic nerve or root pathology. Sciatica symptoms can occur from pathology occurring anywhere along the course of the sciatic nerve, the most common cause being a herniated lumbar intervertebral disc.In older patients, lumbar spinal stenosis may cause sciatica symptoms.
Sciatica is a clinical diagnosis based on the presence of radiating pain in one leg, with or without the associated neurological deficits of parasthesia and muscle weakness. Sciatica pain is often worsened with flexion of the lumbar spine, twisting, bending, or coughing.
Anatomy
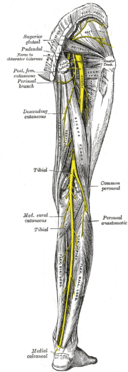
The sciatic nerve is made up of the L4 through S3 nerve roots which coalesce at the pelvis to form the sciatic nerve. At up to 2 cm in diameter, the sciatic nerve is easily the largest nerve in the body.
The sciatic nerve provides direct motor function to the hamstrings, lower extremity adductors, and indirect motor function to the calf muscles, anterior lower leg muscles, and some intrinsic foot muscles.
Indirectly through its terminal branches, the sciatic nerve provides sensation to the posterior and lateral lower leg as well as the plantar foot.
Etiology
Any condition that may structurally impact or compress the sciatic nerve may cause sciatica symptoms.
Sciatic nerve injury can also result in sciatica symptoms (such as pain, muscle weakness and paresthesia) and is usually caused by a traumatic injury (pressure, stretching or cutting), rather than compression or irritation of the nerve. Please read our sciatic nerve injury page for more information.
The causes of sciatica can be categorised into spinal or non-spinal causes or iatrogenic.
Spinal causes:
- Spinal stenosis (due to degenerative bone disorders, trauma, inflammatory disease)
- Spondylolisthesis
- Herniated or bulging lumbar intervertebral disc
- Spinal or paraspinal mass (malignancy, epidural hematoma or abscess)
Non Spinal causes:
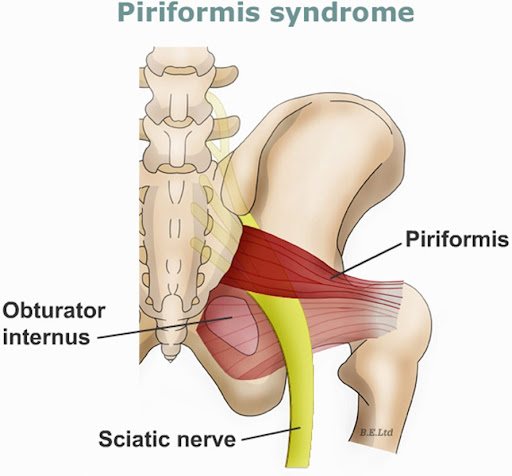
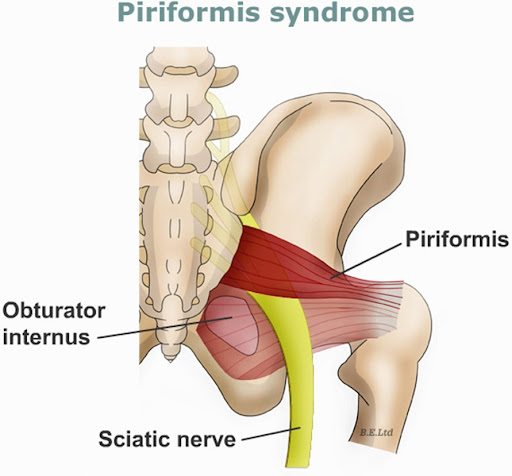
- Piriformis syndrome
- Pregnancy
- Lumbar Radiculopathy
- Pelvic tumours
- Trauma to leg
Iatrogenic causes:
- Direct surgical trauma
- Faulty positioning during anaesthesia
- Injection of neurotoxic substances
- Tourniquets
- Dressings, casts or faulty fitting orthotics
- Radiation
Clinical Presentation
Patients with sciatica can present with neurological symptoms such as:
- Radicular pain in the distribution of the lumbosacral nerve root
- Sensory impairment/disturbance, such as hot and cold or tingling/ burning sensations in the legs or numbness
- Muscular weakness
- Reflex impairment
- Gait dysfunction
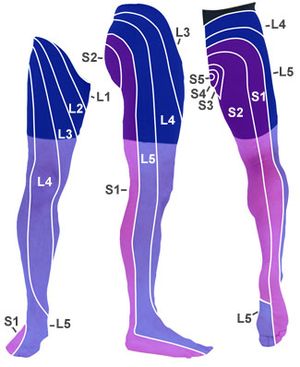
Sciatica symptoms of paresthesias or dysesthesias and oedema in the lower extremity can differ, depending on which nerve is affected.
- L4: When the L4 nerve is compressed or irritated, the patient feels pain, tingling and numbness in the thigh. The patient also feels weak when straightening the leg and may have a diminished knee jerk reflex.
- L5: When the L5 nerve is compressed or irritated, the pain, tingling and numbness may extend to the foot and big toes.
- S1: When the S1 nerve is compressed or irritated, the patient feels pain, tingling and numbness on the outer part of the foot. The patient also experiences weakness when elevating the heel off the ground and standing on tiptoes. The ankle jerk reflex may be diminished.
Differential Diagnosis
A thorough differential list is important in considering a diagnosis of sciatica and should include:
- Herniated lumbosacral disc
- Cauda Equina syndrome
- Muscle spasm
- Nerve root impingement
- Epidural abscess
- Epidural hematoma
- Tumor
- Potts Disease, also known as spinal tuberculosis
- Piriformis syndrome
Evaluation
Sciatica is most commonly diagnosed by:
History:
Complaints of radiating pain in the leg, which follows a dermatomal pattern.
- Pain generally radiates below the knee, into the foot.
- Patients complain about low back pain, which is usually less severe than the leg pain.
- Patients may also report sensory symptoms.
Special tests:
Clinicians should always look for and inquire about red flags when evaluating sciatica or in patients who present with any low back pain. Patients with signs of urinary retention or decreased anal sphincter tone should be urgently referred for investigation as this suggests cauda equina syndrome.
- Lasègue’s test
Also called as straight leg raising test (SLR) is the most commonly performed physical test for diagnosis of sciatica and lumbar disc hernia . The SLR is considered positive when it evokes radiating pain along the course of the sciatic nerve and below the knee between 30 and 70 degrees of hip flexion. Studies of its capacity to diagnose lumbar disc hernia show high sensitivity but low specificity.
Physical Therapy Management
In most cases of sciatica, conservative treatment is favoured. The evidence does not show that one treatment is superior to the other.
Patient Education: to include information on the nature of low back back, advice on self-management techniques and encouragement to continue normal activities.
Promote self management techniques such as:
- use of hot or cold packs for comfort and to decreased inflammation
- avoidance of inciting activities or prolonged sitting/standing
- Regularly changing position i.e. from sitting to standing
- practicing good erect posture
- use of proper lifting techniques
Exercise:
exercises to increase core strength, gentle stretching of the lumbar spine and hamstrings, regular light exercise such as walking, swimming, or aquatherapy
Manual therapy: spinal manipulation, mobilisation or soft tissue techniques such as massage - used alongside exercise and patient education
Here are 10 key physiotherapy interventions for sciatica:- Sciatic Nerve Glides/Flossing: Gently moves the nerve back and forth to reduce sensitivity, often performed by laying on the back, pulling the knee toward the chest, and extending the leg.
- McKenzie Prone Extension (Cobra Stretch): Lying on the stomach and slowly rising onto elbows or hands to extend the lower back, which helps push back bulging discs that cause sciatica.
- Piriformis Stretch: Stretching the piriformis muscle in the buttock, which can compress the sciatic nerve, often done by pulling the knee toward the opposite shoulder while lying down.
- Pelvic Tilts: Strengthening the lower abdominals by tightening the belly and flattening the back against the floor, reducing lower back strain.
- Sitting Spinal Stretch (Spinal Twist): Sitting on the floor with legs extended, crossing the affected leg over the other, and turning to stretch the lower back.
- Knee-to-Chest Stretches: Pulling one or both knees to the chest while lying on the back to increase flexibility in the lower back.
- Child’s Pose: A resting position that stretches the lower back muscles, helping to create space in the lumbar spine.
- Bridge Exercise: Lifting the hips while lying on the back with knees bent to strengthen the glutes and lower back, stabilizing the spine.
- Manual Therapy/Soft Tissue Mobilization: Hands-on treatment by a therapist to release tension in the muscles and improve joint mobility in the spine.
- Heat/Cold Therapy: Applying hot packs to reduce muscle spasm or cold packs to reduce inflammation, often used before or after stretches.